Evaluation and Surgical Management of Chronic Venous
Insufficiency
Charles O. Brantigan MD FACS
The sores of poor people....are often mended by rest, a
horizontal position, fresh provisions and warmth in hospitals...John
Hunter
Venous reconstructive surgery is one of the new and particularly
interesting aspects of vascular surgery. The generally satisfactory
results of compression therapy for venous insufficiency, however,
limits the number of patients for whom surgical reconstruction is an
appropriate option. As a result, the number of venous reconstructive
cases seen in any large vascular surgical practice is similarly
limited. My goal in this presentation is to discuss the physiology
of the venous system, available tests of venous physiology, and
consider the role of venous reconstruction and destruction in the
management of the postphlebitic leg. This discussion is limited, by
necessity, by lack of large numbers of cases or extended follow up
in mine or reported series.
The physiology of the post-phlebitic leg is reasonably well
understood, although there are uncertainties as to the best way to
quantify the magnitude of the disorder. Obviously any operation for
arterial or venous disease must be based on an understanding of the
pertinent physiology. Clearly, not all anatomically demonstrable
lesions either on the arterial or venous side need to be repaired.
In order to define a rational treatment plan, the physiology of
chronic venous insufficiency must be considered on both a macro and
a micro basis.
On a macro basis, one must begin with the anatomy of the lower
extremity and consider, in descriptive terms, what components make
up the venous system, and how each contributes to its overall
function.
There are three venous systems in the leg, the superficial veins,
the deep veins, and the perforator veins. Each has a different
function. The superficial veins collect blood from the skin
subcutaneous tissue and from the foot and convey it to the deep
system. Preferential drainage of the foot into the superficial
system explains why edema of the foot is a common complication of
saphenous vein harvest. The superficial system is made up of
collecting veins and the greater and lesser saphenous veins. All of
these veins are protected by one way valves insuring flow in the
proper direction. The blood collected in the superficial system
either drains through the perforating veins into the deep system or
directly from the greater and lesser saphenous veins into the
femoral or popliteal veins respectively. The perforating veins are
protected by one way valves which insure flow into the deep system.
Generally speaking, the perforating veins are small and cannot be
well visualized either on venography or using duplex scanning. The
deep system serves as a pump conveying blood through a low pressure
system against the force of gravity and into the heart. There are
multiple veins within the soleus and gastrocnemius muscle, in
particular, which serve as collecting chambers. These soleal sinuses
passively fill with blood while the calf muscle is relaxed. When the
calf muscle contracts, blood is forced out of the soleal sinusoids
into the tibial veins and from thence uphill . Retrograde flow is
prevented by the presence of one way valves. This pumping mechanism
allows blood to flow uphill against gravity in spite of the fact
that pressure in the system is less than the hydrostatic forces
imposed by gravity.
|
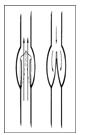
Normal function of venous valve--open when flow is forward,
closed to prevent retrograde flow. |
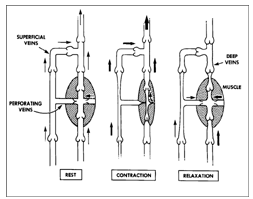
Function of the calf muscle pump during a complete cycle of
relaxation, contraction and relaxation. One way valves direct
flow upward against gravity. From Sumner, DS, OP, CIT |
As can be presumed by this functional anatomic description, there
are only two things that can go wrong with the venous system: One or
more of the veins can become obstructed, or segments of the system
can become incompetent. Incompetence and/or obstruction lead to
venous hypertension, and venous hypertension leads to the post
phlebitic leg.
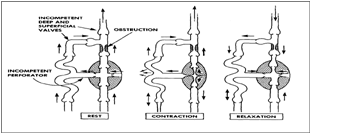
The abnormal calf pump. There is deep vein obstruction and
valvular incompetence. With contraction blood is forced toward
the skin. From Sumner, op cit
The incidence of post phlebitic changes in venous stasis ulcers
is roughly related to the pattern of disease which is, in turn,
roughly related to the degree of venous hypertension which can be
measured directly. The data in the associated tables, modified from
Dr. Browse's work is particularly valuable in answering questions
concerning the prognosis of patients with chronic venous
insufficiency.
Venous Disorders of the Legs
Pathology, Ambulatory Pressure and Ulceration
(modified from various papers by Browse)
| Condition |
Pressure
c cuff |
Pressure
s cuff |
Incidence ulceration |
|
| Normal |
20 mmHg |
20 mmHg |
none |
| Primary |
20 mmHg |
30 mmHg |
1% |
| Varicose Veins |
|
|
|
Varicose Veins
Incompetent Perforators |
50 mmHg |
60 mmHg |
10% |
| Deep Vein Incompetence |
70 mmHg |
70 mmHg |
50% |
Proximal. Occlusion
competent valves |
50 mmHg |
50 mmHg |
15% |
Incompetence and
obstruction |
100 mmHg |
100 mmHg |
80% |
|
On a micro, or cellular level, the pathophysiology of the venous
stasis ulcer has been explained by multiple theories. The most
credible theory is the one expounded by Browse . He postulated that
venous hypertension causes leaky vessels through separation of
endothelial cells. Relatively low degrees of separation produce
extravasation of fluid. As the pressure becomes higher, the pores
become relatively larger, and larger things are extravasated,
eventually large proteins such as fibrinogen, and eventually red
cells. The red cells decompose in the extravascular space, releasing
hemoglobin pigment. This eventually becomes the hemosiderin which
discolors the affected area in most patients with the postphlebitic
leg. The fibrinogen is polymerized into fibrin and this fibrin coats
the capillaries surrounding the areas most affected by high
pressure. These fibrin cuffs have been demonstrated microscopically
by selective staining. The effect of coating the capillaries is to
decrease diffusion of oxygen across cell membranes. This means that
the capillary bed serves functionally as a shunt, conveying blood
without transporting oxygen. This makes the venous effluent from the
area of a venous stasis ulcer abnormally high in oxygen content. The
resulting tissue hypoxia stimulates new vessel formation. The new
vessels eventually become coated with fibrin as well. Thus, an
ischemic ulcer is created in the presence of exuberant capillary
proliferation and increased oxygen tension. There is an intense
fibrotic reaction both to the deposition of fibrin and the
deposition of hemosiderin pigment leading to the badly damaged and
fibrous appearing tissue that appears under the bleeding base on the
venous stasis ulcer. In addition, for some unknown reason, these
patients have a deficit of naturally occurring fibrinolytic activity
in the area of the ulcer, and this encourages deposition rather than
dissolution of fibrin.
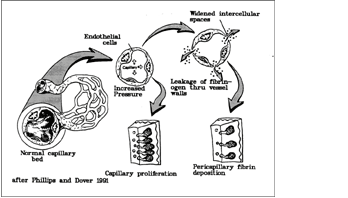
The Browse theory of pathogenesis of venous stasis
ulceration.. See text.
If we are to deal with chronic venous insufficiency on a surgical
basis, we must begin by correcting problems of venous incompetence
and obstruction. Before we can correct them, we must identify the
location of obstructions and incompetent valves. Many tests have
been proposed for the evaluation of venous stasis disease. Each test
is, of course, embraced enthusiastically by its advocate. Instead of
discussing all available tests, I prefer to discuss the tests which
have proven valuable to us in Denver.
To begin with, many venous tests are too imprecise to provide
much help in evaluating the post phlebitic leg. Certainly, impedance
plethysmography and radioisotope venography are basically useless in
planning possible surgical therapy. Our experience has been that
venous reflux testing, although widely advocated, produces such
variable results that it is of no value either. We rely on Color
Duplex Scanning and ascending and descending venography to make
surgical decisions, although we are still not sure how to deal with
the discrepant data which is occasionally produced by the three
tests.
We begin our evaluation with Color Duplex Scanning. In most
patients the most accurate evaluation of the patency of the venous
system, including the tibial veins and the perforators, is
accomplished in this way. In order to accomplish this, however,
state of the art equipment is required, well trained and interested
technologists, and more time than will ever be paid for by insurance
companies, or particularly, by Medicare. Although there are
technical limitations to the study, primarily due to obesity or
massive edema, in most patients we can see and evaluate the six
named tibial veins and the venous system up to and through the
external iliac vein. Information about the common iliac vein and the
vena cava is attainable as well, although it appears to be somewhat
less reliable. Color Duplex Scanning appears to be our most
important test because we are able to determine which segments are
occluded and which segments are incompetent. Considerable experience
is required, however, because many times following deep vein
thrombosis, the occluded segments become partially recanalized and
it is then up to the technologist to determine if the vein is still
functionally occluded. When we are able to visualize specific venous
valves, it makes an impressive picture which displays well at
meetings. Unfortunately, however, we are generally able to
demonstrate venous valvular competence or incompetence by the
absence or presence of venous reflux seen using the low flow
settings of the Color Duplex Scanner.
It must be noted that Duplex Scanning provides information about
the superficial system and the perforating veins which is available
in no other way. Contrast venography is generally carried out by
obstructing flow through the superficial system in order to force
the dye into the deep system. As a result, the opacification of the
saphenous veins generally occurs only through incompetent
perforators. Likewise, since there are many incompetent perforators,
they can be identified with contrast venography, but not with the
precision required to specifically interrupt these perforators using
limited incisions.
Ascending venography is useful in that it provides an anatomic
roadmap of the entire deep venous system. Contrast venograms are
generally assigned to the lowest level of radiology resident and are
often do not provide the amount of information that could be
provided had they been done by someone who understood the importance
of visualizing all tibial veins and visualizing the iliac veins as
well. Successful surgery requires a quality roadmap. Ascending
venography also provides us with roadmap information concerning the
location of venous valve sinuses which, in turn, allows us to
identify valve sinuses which we may not be able to see grossly at
the time of surgery when the veins are not distended.
Descending venography is accomplished by introduction of dye into
the iliac vein from above and watching the progress of its reflux
down the leg . The degree of reflux is generally measured using the
Kistner classification. Descending venography is also useful in
identifying valve sinuses for possible surgical repair. The valve
cusps which are incompetent are commonly identified in descending
venography and provide some information to the surgeon concerning
the most likely valve cusp to repair.
|
Descending Venography
Kistner Classification |
| Grade 0 |
Competence |
No reflux below
common femoral |
| Grade I |
Minimal
Incompetence |
Reflux to upper
thigh |
| Grade II |
Mild Incompetence
|
Reflux to just
above knee |
| Grade III |
Moderate
Incompetence |
Reflux to level
of knee |
| Grade IV |
Severe
Incompetence |
Reflux to calf
veins |
|
It is important to remember that the duplex scan and the contrast
studies must be used together. Recanalized veins pose particular
problems in evaluation. This recanalization often occurs in a
sponge-like fashion which can be characterized as cavernous
transformation. A vein that has undergone cavernous transformation
will often be identified on ascending venography as an open vein and
on descending venography as a competent vein when, in fact, the vein
is functionally occluded. Making this assessment on duplex scanning
is not easy, but it is more precisely done than with contrast
studies.
Surgical modalities of interest in the management of the post
phlebitic leg are many and varied. Each appears to have its own
usefulness. Beginning with the most simple and proceeding to the
most complex, I would like to comment on the role of the various
surgical techniques.
Ligation and stripping of incompetent varicose veins is a time
honored treatment. Unfortunately, it is commonly considered
primarily for patients who have cosmetic problems or aching and
swelling associated with varicose veins and is seldom considered as
part of the treatment for patients with a post phlebitic leg. A
surgical attack on the superficial system, when carried out, needs
to be done completely. Ligation and stripping of the greater
saphenous vein is often not sufficient. Secondary veins should be
obliterated as well. Particular attention must be paid to the
posterior arch vein, when present. It begins behind the medial
maleolus and extends upward to join the greater saphenous vein below
the knee. The lesser saphenous vein should be removed when it is
incompetent, and the number and severity of scars made on the leg to
achieve ligation and stripping of the superficial system in the
context of the chronic venous ulcer is less important than it is in
young women with a cosmetic problem or swollen legs. Operating on
the patient with the leg elevated will markedly decrease the blood
loss associated with these procedures, and some surgeons have even
advocated using a tourniquet for hemostasis as one works through
multiple incisions below the knee. Obviously, destruction of the
incompetent portions of the superficial system will be effective in
treatment of venous disease only if physiologic studies demonstrate
that it is the principal defect. This occurs on occasion, but it is
uncommon. There is a role for such destruction of an incompetent
superficial system in the presence of deep vein incompetence, but
its role in patients who have an obstructed deep system is
uncertain, and according to some reporters, contraindicated.
Interruption of perforators has been carried out in the past
using the Linton flap procedure or similar procedures . In my
opinion, this procedure is outmoded and has no place in clinical
medicine because of the massive nature of the operation and the high
incidence of wound healing complications which are associated with
it. Interruption of perforators is important, however. The
perforators are generally marked using Duplex Scanning and are
interrupted by making a number of small incisions under local
anesthesia directly over the perforator. The perforator is
identified where it comes through the fascia and is ligated in a
subfascial manner. Again, if the patient's only problem is an
incompetent perforator, then ligating the perforator under local
anesthesia and day care surgery will be of great physiologic
benefit. The role of the SEPS procedure or subfascial endoscopic
perforator ligation remains to be determined. The procedure has some
usefulness, but is limited by subcutaneous fibrosis in severe cases
and by the location of the perforators in others.
Ligation of an incompetent profunda femoris vein can be immensely
beneficial to some patients. In some patients, descending venography
will show that the superficial femoral vein (part of the deep
system) is competent but that the profunda femoris vein is
incompetent and feeds incompetent perforators below the knee. It is
difficult to thoroughly evaluate the profunda femoris vein using
Duplex Scanning. In addition, there may be more than one profunda
femoris vein, and ligation of the wrong one will not produce any
benefit. Likewise duplications in the deep system will occasionally
be identified in which one limb is incompetent and the other limb
competent. In this case, ligation of the incompetent limb will
markedly improve the patient's physiology.
In some patients with an incompetent venous system, it is
possible to identify a venous valve either in the profunda femoris
vein or in the greater saphenous vein which is competent. It is a
relatively straightforward surgical procedure to transpose this
valve into the incompetent superficial femoral vein . Our experience
has been that these transposed valves tend to fatigue with time.
Particularly if the patient is non compliant with the need for
elastic support stockings in the postoperative period, venous valve
fatigue will be a common problem. We use a wide mesh Dacron fabric
to wrap these transposed valves, as our experience has shown that
one of the common ways that these valves fatigue is for the
transposed segment is to dilate making the annulus larger and the
valve incompetent. Note that use of wide mesh material rather than a
section of a vascular graft is selected because it offers less
resistance to ingrowth of blood vessels into the vein itself.
Venous valve transplantation, as proposed by Taheri , has been
successful in selected patients. In this procedure a competent
venous valve is identified from elsewhere, generally one of the
duplicated axillary veins. The valve bearing segment of vein is then
excised and transplanted into the deep system of the leg. The size
match is generally best in the popliteal vein. When we performed
this operation, we prefer to reinforce the transplanted segment with
wide mesh Dacron fabric for the same reason that we reinforce
transposed valves.
Venous valve repair, as proposed by Kistner , has been our most
reliable technique. The venous valves are then repaired directly by
plicating either the annulus or the valve leaflet itself using
magnification. The technical details are described in Kistner's
articles, but resemble an annuloplasty of the tricuspid valve. We
prefer to reinforce the plicated valve with Dacron mesh because of
problems of dilation of the annulus. Our patient population must be
significantly different from that of Kistner's, reflecting a higher
incidence of post phlebitic legs rather than patients with primary
valvular incompetence. In our experience, a relatively small number
of patients have been candidates for this procedure.
Valve repair. Use of micro sutures to
tighten leading edge of valve
Bypassing obstructed venous segments can be carried out as well.
The time honored operations, the Palma crossover procedure and the
Husni saphenopopliteal bypass , are not procedures that we have had
a great deal of experience with. While many physicians have reported
good results with these operations, their role is yet to be defined.
There is some question about whether they should be "protected" by
doing a simultaneous AV fistula which is subsequently ligated. There
is usually little morbidity associated with these procedures even if
they fail.
Our best results with obstructed veins has been to use the spiral
vein graft . This technique appears to be particularly useful in
bypassing an obstructed iliac vein segment or a superficial femoral
vein segment. This is a tedious and time consuming procedure whose
charm will decrease in our eyes as soon as other people are willing
to invest the time and effort required to construct these conduits.
We are currently investigating the use of cryopreserved iliac veins
for these conduits.
Patient selection for evaluation and for vascular surgical
procedures on the venous system is complicated. My own inclination
is to say that everyone with a post phlebitic leg who has stasis
pigmentation or ulceration should undergo a complete evaluation, at
least using Duplex Scanning. There will be a significant number of
patients discovered whose problem is principally an incompetent
superficial system and/or incompetent perforators. Since ligation
and stripping of the superficial system is a relatively
straightforward operation with a long, successful track record, I
would be inclined to recommend this operation for whom the primary
cause of their venous stasis ulcer is incompetence of the
superficial system. Likewise, when patients have a prominent problem
with incompetent perforators, ligation of these perforators under
limited anesthesia using limited incisions will make a significant
improvement in the patient's physiology and should be considered in
most patients. Destruction of the superficial system in the face of
deep system incompetence is a judgement call based on the surgeons
assessment of the relative contribution of each component and I am
unable to provide specific guidance in making this judgment.
On the other hand, the various venous bypass procedures and valve
reconstructions should be considered in patients whose problems and
symptoms are refractory to good elastic compression care, for
patients for whom elastic support is not a consideration, or for the
occasional patient with venous claudication. As with arterial
disease, chronic venous insufficiency is an ongoing process, and
there are many more things that can go wrong in the post operative
patient who has venous disease than in one who has arterial disease.
Since elastic compression is the most important way of preventing
many of these problems, all postoperative patients are advised to
wear elastic compression stockings for the rest of their lives.
Under these circumstances, it is sometimes difficult to determine
whether the patient's improvement following venous surgery is the
result of more compulsive attention to elastic compression, or
whether the patient is benefiting from the operation. Obviously if
patients are required to wear elastic support post operatively, most
of the surgical options are not appropriately offered to patients
whose symptoms are already controlled with elastic support. In
addition, the durability of these repairs and the long term results
are not well known because the numbers of patients upon whom they
have been performed is small and long term follow up is incomplete.
The surgical management of venous disease is particularly
rewarding for the interested physician. The physiology is complex
and fun to elucidate. Patients respond well to therapeutic regimens
which are well conceived and well carried out, and the patients,
particularly ones who have had long standing venous stasis ulcers,
are very grateful when the problem is solved.
Dr Brantigan wrote the original version of this paper in 1992 and
has presented this information at many medical meetings. This
version was created in 1998 as a syllabus for such a presentation.
References:
1 Hunter, J Palmer, JF (ed) The works of John
Hunter. London, Longman, Reese, Orme, Brown, Green and Longman 1837
2 Lofgren, EP, Myers, TT, Lofgren, KA, Kuster, G,
The Venous Valves of the Foot and Ankle, Surg Gynec Obstet 289-290
(1968). Reese, Orme, Brown, Green and Longman 1837
3 Lofgren, EP, Myers, TT, Lofgren, KA, Kuster, G,
The Venous Valves of the Foot and Ankle, Surg Gynec Obstet 289-290
(1968).
4 Criado, E, Johnson, G, Jr, Venous Disease,
Current Problems in Surgery XXVIII (5) May 1991 p345.
5 Sumner, DS, Venous dynamics--varicosities,
Clinical Obstet Gynec 24:743-760 (1981)
6 Browse, NL, The pathogenesis of venous
ulceration, in Bergan, JJ and Yao JST, Surgery of the veins, Grune
and Stratton, New York 1985 p25 ff.
Taheri, SA, Sheehan, F, Elias, S, Descending
Venography, Angiology 34: 299-326 (1983).
7 Kistner, RL, Ferris, EB, Randhawa, G, Kamida, C,
A method of performing descending venography, J Vasc Surg 4:464-8
(1986).
Linton, RR, Postthrombotic ulceration of ht lower
extremity: Its etiology and surgical management, Ann Surg 138:415-32
(1953).
8 Queral, LA, Whitehouse, WM Jr, Flinn, WR, Neiman,
HL, Yao, JST, Bergan, JJ, Surgical correction of chronic deep venous
insufficiency by valvular transposition, Surgery 87:688-695 (1980).
9 Meadox Dacron Mesh catalog number 019206
10 Taheri, SA, Lazar, L, Elias, S, Marchand, P,
Heffner, R, Surgical treatment of postphlebitic syndrome with vein
valve transplant, Am J Surg 144:221-224 (1982).
11 Kistner, RL, Surgical repair of the incompetent
femoral vein valve. Arch Surg 110:1336-42 (1975).
12 Bergen, JJ, Yao, JST, Venous Problems, Yearbook
Medical Publishers, Inc, 1978.
13i Palma, EC, Esperon, R, Vein transplants and
grafts in the surgical treatment of the postphlebitic syndrome, J
Cardiovasc Surg 1:94-107 (1960).
14 Husni, EA, In situ saphenopopliteal bypass graft
for incompetence of the femoral and popliteal veins, Surg Gynec
Obstet 130:279 (1970).
15 Smith, ER, Brantigan CO, Bypass of superior vena
cava obstruction using spiral vein graft, J Cardiovasc Surg
24:259-61 (1983). |